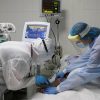
More than 90% of COVID-19 patients take antibiotics, not only in hospitals, but also on an outpatient basis, according to Roman Kozlov, chief microbiologist and antimicrobial resistance specialist at the Russian Ministry of Health, an associate member of the Russian Academy of Sciences. This results in resistance of bacteria to medications. Because of it, people may encounter infections that they would not be able to overcome. Biologist Aleksander Panchin and therapist Aleksander Melnikov told Pravmir why antibiotics should not be taken “just in case” and why they are dangerous.
More than 90% of COVID-19 patients take antibiotics, not only in hospitals, but also on an outpatient basis, according to Roman Kozlov, chief microbiologist and antimicrobial resistance specialist at the Russian Ministry of Health, an associate member of the Russian Academy of Sciences. This results in resistance of bacteria to medications. Because of it, people may encounter infections that they would not be able to overcome. Biologist Aleksander Panchin and therapist Aleksander Melnikov told Pravmir why antibiotics should not be taken “just in case” and why they are dangerous.
Aleksander Panchin, a Russian biologist, popularizer of science, explains why resistance to antibiotics is horrible and debunks myths about them.
— Why is it so horrible that many people take antibiotics now? What is resistance? Will they stop helping me personally?

Aleksander Panchin
— A bacteria and not a person can have resistance to antibiotics.
Even before you start taking an antibiotic, your body may have bacteria that are more or less resistant to this antibiotic.
Where does resistance come from? Natural resistance to different antibiotics occurs to different degrees in different bacteria. When we take antibiotics in large numbers without thinking, we conduct artificial selection in favor of those varieties of bacteria that are more resistant.
Some mutations that affect resistance, some variations of it are present in the bacterial population by definition. But the longer we subject them to such artificial selection, the easier new mutations become permanent.
The more frequently and massively we use antibiotics, the more resistant bacteria there will be, and the less effective antibiotics will be in the future.
The world health organization (WFO) warns that antibiotics are a resource that we can run out of if we use them carelessly. If we are too wasteful in using antibiotics, then at some point it may turn out that the usual bacterial infection, which was previously easily overcome with their help, is now becoming dangerous for humans.
We know examples of quite dangerous resistant strains of bacteria that cannot be treated with any kind of antibiotics, in general. For example, Staphylococcus aureus.
Resistance to antibiotics is one of the most serious threats to human health today. More and more infectious diseases, such as bacterial pneumonia, tuberculosis, gonorrhea, and salmonellosis, are becoming more difficult to treat because of the reduced effectiveness of these medications.
Longer hospitalizations, increased medical costs, and increased mortality are the consequences of the bacterial resistance to antibiotics.
— Antibiotics treat everything, even COVID-19. Are they helping so far?
— No. Antibiotics are medications for bacteria. They do not help with viral diseases, including COVID-19.
Bacteria are very different. They are genetically different from each other within the same strain. Therefore, their resistance to antibiotics is different.
Bacteria have a variety of mechanisms that help them protect themselves from antibiotics. They prevent the medication from entering the bacteria, pump the antibiotic out of bacteria, destroy it, and so on. Different bacteria exercise these mechanisms to different extents, and resistance develops to different antibiotics.
When we use some antibiotic, then those bacteria, which do not have these mechanisms developed, die. Those bacteria that have the ability to survive in the presence of this antibiotic due to some genetic mutations can pass these genetic variants of resistance to next generations of bacteria, to their descendants.
The most unpleasant thing is that the so-called horizontal gene transfer is well-developed in bacteria. They can exchange genetic material among themselves.
Even if these bacteria are not very related, they can exchange plasmids, for example. Plasmids are circular DNA molecules. Some of the antibiotic resistance genes may be on these plasmids. And an antibiotic-resistant bacterium passes these plasmids to a non-resistant bacterium, and it becomes insensitive to the antibiotic.
Therefore, doctors prescribe certain antibiotics based on the diagnosis. Because different bacteria cause different bacterial diseases.
Taking antibiotics “just in case” is dangerous
— Can people take antibiotics to prevent diseases? Just in case, so as not to get sick.
— COVID-19 is caused by a virus. Antibiotics do not work on viruses, so taking them to treat coronavirus and even more so for prevention is a pernicious idea. Both for a specific patient and due to the development of mass resistance of bacteria to antibiotics, in general.
It is necessary, however, to caveat that there are bacterial complications associated with a viral infection. In this case, if a doctor suspects that a person has such complications, they can prescribe antibiotics. The doctor bases the prescription of a specific antibiotic, its administration period and dose on modern scientific research and symptoms. The doctor should take all this into account.
When people prescribe antibiotics for themselves, they often do not need them. In this case, they can only be harmful.
It is pointless to take antibiotics for prevention. Except for cases when doctors prescribe them before some operations.
It is a separate problem when people, who prescribe antibiotics for themselves, take them incorrectly. In this case, it is bad to both underuse and overuse them.
It is bad to underuse them because you do not finish off the bacteria, you think that you got better, but the bacteria did not go away. It is also bad to overuse them because you have already killed the bacterium, but continue to take an antibiotic, and this only contributes to other bacteria, which may be in your body, developing resistant strains. They may even be non-pathogenic bacteria but they transfer the resistance to some pathogenic ones. You are harming yourself: bacteria in your body become more resistant.
The problem of bacterial resistance to antibiotics is not limited to humans. Antibiotics are sometimes also used excessively in animal agriculture. The problem is not that it somehow negatively affects the quality of meat products, or something like that. No. The problem is that there is more and more resistance.
If people stop overusing antibiotics en masse, then the developed resistance mechanisms in bacteria may decrease over time.
— I was afraid I would get sick, so I have bought a stock of antibiotics. Shouldn’t I have?
— You should not have. After all, antibiotics are usually given with prescription, and this is the way it should be.
You should clearly understand that if you take antibiotics without a doctor’s prescription, you bring the post-antibiotic era closer. It is when almost overcome infections and minor injuries can become fatal again.
To date, there are no medications that have proven to be effective against SARS-CoV-2 coronavirus, the causative agent of COVID-19, according to WHO.
Unfortunately, people in our country are prescribed a lot of ineffective or questionable medications.
WHO holds an annual week of proper antibiotic use under the slogan “Antibiotics: use carefully!” Here are the main recommendations of the World Health Organization:
- only use antibiotics when prescribed by a certified health professional;
- never demand antibiotics if your health worker says you do not need them;
- always follow your health worker’s advice when using antibiotics;
- never share your antibiotics.
These medications will help not everyone with COVID-19
Alexander Melnikov, a therapist, talks about side effects of antibiotics and why they are often prescribed for treating COVID-19 (sometimes completely in vain).
— I have COVID-19. A doctor prescribed me antibiotics. What should I do?
— You can go to another doctor to get a second opinion as with any other disease. You as a patient have every right to do so.
Unfortunately, the practice of uncontrolled and unjustified use of antibiotics has spread in our country, especially now, during the pandemic. At the same time, antibiotics in large quantities in the COVID-19 environment are both prescribed by doctors and often used by patients themselves.
Many people believe that both the disease itself and lung damage are indications for prescribing antibiotics. This is completely wrong.
— However, doctors recommended antibiotics in the beginning of the pandemic.
— Yes, but that does not mean that everyone should take them.
Of course, a person can have a variety of bacterial infections, when they need to use antibiotics. For example, for bacterial pneumonia that is quite common. And for other infections, there are many of them, when doctors often prescribe such medications.
As for the use of antibiotics for treatment of the coronavirus infection, we are all thinking now why people started taking them. This is usually associated with bacteria “gravitating” to the viral lesion quite easily during such a common viral infection like flu, which can also lead to severe lung damage. When the pandemic first broke out, it was assumed that the same would happen for COVID-19, and serious experts widely recommended the use of antibiotics for treating coronavirus infection.
Then it turned out that bacterial infection during COVID-19 occurs for certain, not yet fully understood reasons. And not very often: according to rough estimates, it occurs in 7-8% of cases and, as a rule, in severe cases, especially in patients on a ventilator. In these cases, it is resistant strains of bacteria that attach most often. And it is then when doctors prescribe antibiotics.
But this is only in hospitals. There is usually no need to use antibiotics on an outpatient basis.
There is another story with Azithromycin, a popular antibiotic, to which some experts attributed not only antibacterial, but also anti-inflammatory properties and effectiveness in COVID-19 treatment. The effectiveness was not confirmed in clinical practice.
— If I take antibiotics in advance, I will not have any bacterial infections, will I?
— This is not true (according to WHO. – Ed.).
A bacterial infection may surely develop, and it can be caused by types of bacteria that are resistant to these antibiotics.
For example, you take antibiotics without a doctor’s prescription. Then, when you develop a bacterial infection, the bacteria will not be sensitive to the medications that you unreasonably took.
It is impossible to prevent a bacterial infection with such a “preventive” method. Bacterial resistance to antibiotics has been observed since antibiotics first appeared in medical practice. Bacteria developed resistance all the time and became insensitive: first to penicillin, then to its derivatives and to all other antibiotics that people synthesized all the time to overcome this.
Bacteria gradually develop resistance to everything. People will create new antibiotics all the time. Sometimes a person has to use three or four antibiotics at the same time to overcome this resistance.
Now people take antibiotics, in part unreasonably, in huge quantities because of the pandemic. And this may be one of the most unfortunate consequences of the pandemic: bacteria increase their resistance.
What side effects do antibiotics cause?
— Yet, antibiotics will not make everything worse, right?
— Quite the opposite. Antibiotics cause various side effects, many of which are rather dangerous.
The side effects include allergic reactions, up to anaphylactic shock. The most common side effect is an antibiotic associated diarrhea, which is caused by normal intestinal flora dying under the influence of antibiotics.
Antibiotics inhibit the development of bacteria or kill them. They also affect the living organism, in which these bacteria are located.
Other flora may develop due to this and it can be very dangerous: for example, clostridium that cause pseudomembranous colitis, which can lead to death.
Antibiotics can negatively affect the liver, activate the development of fungal flora, suppress hematopoiesis, affect the central nervous system, and so on. They should be used like any other active medication in cases when the potential benefit of their use exceeds the possible harm.
Antibiotics will not be beneficial for COVID-19 treatment, and the harmful side effects of using them are quite real.
— Since antibiotics have so many side effects, I will not give them to my children.
— There are situations when antibiotics are absolutely necessary for children.
For example, bacterial streptococcal angina. This is a bacterial infection that is quite dangerous. It can cause damage to the heart valves and lead to heart defects.
If it is a bacterial infection, then you need to take antibiotics. There is no big difference in their administration for children and adults.
Translated by Julia Frolova